Digestive
This resource provides current and comprehensive health care information for school health nurses. Related procedures, instructional videos and downloadable skills checklists can be searched by selecting the [More Information] button at the bottom of this web page.
Overview
Indication for Use:
Gastrostomy tubes are indicated for children who have a functioning gastrointestinal tract but have difficulty ingesting or cannot ingest nutrition orally. Children may require gastrostomy tube feedings for development, mechanical reasons, or secondary to another health condition. Some conditions that may warrant the placement of a gastrostomy tube are:
- Failure to thrive
- Abnormalities of the throat or esophagus
- Swallowing difficulties
- Metabolic conditions
- Nervous system dysfunction (i.e., cerebral palsy)
- Cancer
- Treatment for cancer
(Farou, Lucas, Olympia, 2021).
Types of tubes:
Tubes typically intended for short-term use (usually less than 6 weeks):
- NG: naso-gastric–Go through the nose and end in the stomach.
- NJ: naso-jejunal–Go through the nose and end in the small bowel.
Tubes intended for more long-term use:
- PEG tube: percutaneous endoscopic gastrostomy tube–typically the first type of tube placed when starting enteral nutrition. Surgical placement of the tube is guided by the use of an endoscope. A plastic bumper is placed in the stomach to help the tube stay in place along with a thin plastic disc that is placed outside of the abdomen (Avanos Medical, 2018).
- G-tube: gastrostomy tube–Surgically inserted into the stomach through the abdominal wall and anchored to the peritoneum at the operation site (Anderson & Herring, 2024).
- G-J tube: gastro-jejunostomy tube–Surgically inserted into the stomach with an extension that goes into the small bowel (Schwartz, 2014).
- J-tube: jejunostomy tubes–Surgically inserted directly into the jejunum, which is a portion of the small intestine (Schwartz, 2014).
Image: Tube Feeding
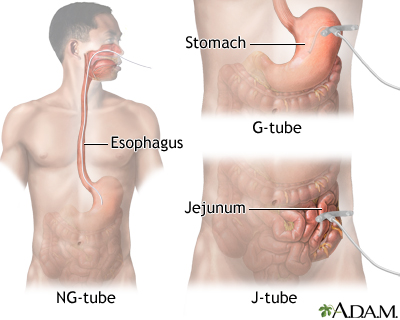
Source: Medline Plus, 2022
Low profile vs. Standard/Traditional Length Tubes:
Low profile device: A low profile device, commonly referred to as a gastrostomy button, rests flat on the skin surface. To access the gastrostomy button during feeds or medication administration, an extension tubing set is used. A low profile tube has a short tube (1 to 5 cm) with an inflatable balloon or “mushroom” bolster inside the stomach or intestine. The capped feeding port is located on the outside of the abdomen (Schwartz, 2014).
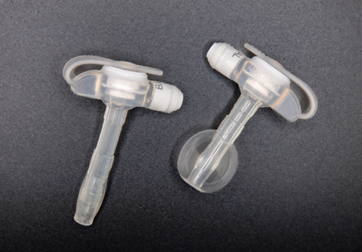
Photo: Low-profile devices with balloons deflated and inflated. (School Health Associates, 2023)
Standard/Traditional length devices: A standard or traditional length device is sometimes referred to as a high-profile device. This device extends off the abdomen about 7-10cm (Applied Medical Technology, 2013). Standard/Traditional length tubes are often used as the initial G-tube for the first 8-12 weeks post-surgery (Feeding Tube Awareness Foundation, 2014).

Photo: Standard length g-tube with bumper and inflated balloon (School Health Associates, 2023).
Possible Complications:
Diarrhea: Diarrhea is a common issue for children with g-tubes and there can be several possible causes, such as liquid food, how fast the enteral feeding is administered, medication, or changes in the normal bacteria in the stomach and intestines. Discuss with the student’s parents/guardians and health care provider, if indicated (University of Chicago Medicine, 2021).
Dislodgement: Dislodgement may occur due to acute trauma, tension along the external tubing, and/or deflation or rupture of the balloon tip. Management of the dislodgement depends on a several factors, including, but not limited to:
- Presence of an order from a health care provider to replace the gastrostomy tube:
- The school nurse would need an order from a health care provider to perform or delegate this procedure to someone else.
- The length of time the gastrostomy tube has been in place:
- Tubes that have been in place for less than 8 weeks should not be replaced in the school setting (Spratling, et al., 2021).
- Type of gastrostomy tube:
- Gastrostomy tubes sutured in place and combined gastrostomy/jejunostomy tubes cannot be replaced in the school setting. The school nurse should develop a plan, in collaboration with the parents and health care provider, regarding what to do if dislodgement of these types of tubes occurs at school (Spratling, et al., 2021).
- Competency of the individual who will be replacing the tube:
- Only individuals who have the knowledge, skills, abilities, and willingness can perform this procedure. If the school nurse does not have the knowledge, skills, and abilities to replace the gastrostomy tube, the school nurse should develop an alternative plan for gastrostomy tube dislodgement.
Granulation Tissue: If granulation tissue continues to grow or becomes irritated, discuss with parents/guardians and health care provider. Medications can be prescribed to help decrease granulation. Hydrogen peroxide should not be used because it may dry the tissue too much leading to additional damage (Anderson & Herring, 2024).
Occlusion/Obstruction: Occlusion or obstruction of the tube can occur when there is solidification of the formula or kinking of the apparatus (Farou, Lucas, & Olympia, 2021). If this occurs, the tube should be flushed with warm water. If the occlusion/obstruction is not remedied with a warm water flush, the school nurse should contact the parents/guardian and health care provider, if needed. Additionally, the school nurse should check the health care provider’s order to determine if other treatments for occlusion or obstruction are prescribed. To help prevent occlusion or obstruction, always flush the gastrostomy tube before and after each medication administration and/or feeding with 5 mL of water or the amount prescribed (Oley Foundation, 2022; University of Chicago Medicine, 2021).
Vomiting: Vomiting could be caused by excessive gas or overfeeding. If vomiting occurs during a feeding, stop the feeding, vent the g-tube by opening the clamp, removing the plug, or opening the end of the g-tube extension set. This could slowly relieve the problem. The vomiting could also be caused if the g-tube has moved forward in the stomach blocking the stomach outlet. The school nurse should follow up with the parents/guardians and health care provider, if indicated (Oley Foundation, 2022; University of Chicago Medicine, 2021).
Delegation
There are a number of factors for the school nurse to consider when deciding whether to delegate this procedure to unlicensed assistive personnel (UAP). This section will provide a list of questions that the school nurse should answer to assist them in determining whether it is appropriate and safe to delegate the procedure. It is also important to remember that the questions related to delegation need to be answered for every individual student. The decision to delegate is based on circumstances related to the student, the nurse, the UAP, and the situation.
Questions to Ask to Inform Safe Delegation: The delegation questions below are based on the American Nurses Association’s Decision Tree for Delegation by Registered Nurses (ANA, 2012).
- Has the school nurse performed an initial assessment of the student to determine their needs?
The school nurse should not delegate the procedure to a UAP until they have completed the initial assessment. - Does school district policy, the school nurse’s job description, and the UAP’s job description allow procedures related to gastrostomy tubes to be delegated?
Although the Missouri Nurse Practice Act allows for registered nurses to delegate gastrostomy tube procedures, the district may have policies that prohibit or limit the school nurse’s ability to delegate. Additionally, the school nurse’s and UAP’s job descriptions may restrict delegation as well. - Is the school nurse competent to perform this procedure or does the school nurse need to acquire some knowledge or skills to be competent in this procedure?
If the school nurse is not competent or does not feel comfortable performing this procedure they should not delegate this procedure to a UAP. The school nurse must first acquire the necessary knowledge and skill to perform this procedure competently before they can delegate it to someone else. - Is the student’s condition stable? Is this an established gastrostomy tube or was it recently placed? How predictable are the outcomes of the procedure?
A school nurse should not delegate tube feedings, medication administration, or care of the gastrostomy tube to a UAP if the student has a newly placed gastrostomy tube. The outcomes are not predictable and thus the school nurse should perform the procedures until the student’s condition has stabilized. - Does the procedure require an initial or ongoing assessment to be performed during the procedure?
If an initial or ongoing assessment is required for the procedure to be performed, the procedure should not be delegated. - Does the UAP have the appropriate knowledge, skills, abilities, and willingness to perform the procedure?
All these factors need to be considered. Although a UAP may be competent to perform the procedure they may not be willing to do so and in that situation another UAP should be identified and trained. The registered nurse must retain responsibility for the procedure until training is complete. - Is there a procedure and/or protocol in place for this procedure?
A delegated nursing procedure must have an established sequence of steps that the UAP can follow. These steps should have a predictable outcome. The steps should be outlined in a written procedure or protocol. If the written procedure/protocol has not been developed, the school nurse should retain responsibility for the procedure until the procedure/protocol is in place. - Is the school nurse able to provide supervision to the UAP (direct or indirect depending on the situation)?
If the school nurse is not able to provide supervision, then the procedure should not be delegated. The school nurse will need to assess the situation to determine if direct or indirect supervision is required. The school nurse may also need to reassess the situation if the environment changes, for example, if the procedure is going to be performed during a time that the school nurse is not contracted to provide nursing services (i.e., over the weekend, during the summer, or if the school nurse is part-time). - Is the student ready to assume some responsibility for the procedure?
The school nurse should resume responsibility for the procedure since the school nurse is the only one who can initiate teaching. The school nurse would also want to observe the student performing the procedure to ensure that the student is competent. Once the school nurse has determined that the student is competent and can safely perform the procedure independently, they can delegate the supervision of the student to a UAP. If at a future date the school nurse is needed to teach the student additional skills, the school nurse would again need to resume responsibility for the procedure until the time in which the school nurse determined the student to be competent.
The Decision to Delegate:
There may be times when the school nurse and school administrator have conflicting opinions on the delegation of a procedure to a UAP. The school nurse may feel that delegation is not appropriate or the administrator may want the school nurse to delegate a procedure to an UAP that the school nurse feels is not competent. In these situations the school nurse may need to educate the administrator that the school nurse has a professional and legal responsibility to determine if delegation of a nursing procedure is appropriate and safe (ANA, 2012). ). See Fact Sheet for School Administrators, Families, and School Personnel: Nursing Delegation Requires the School Nurse and Navigating Delegation in the School Setting (pdf) to assist school nurses communication with the school administration.
School Environment
Space and Time to Perform the Procedure
This procedure requires additional resources including a second person to assist with the procedure, 30 minutes of uninterrupted time, and the ability to perform this procedure using Aseptic non touch technique (ANTT®). If the school nurse does not have the capability to perform this procedure then the school nurse should discuss with the student’s parents/guardians and health care provider to arrange a different plan.
Physical Education and Recess
The school nurse should review the health care provider’s order to see if there are any activity restrictions associated with the student’s central venous line and/or underlying health condition that may require precautions during physical education class or at recess. Many students with CVLs will be advised to not participate in contact sports and use an abdominal binder, ace wrap, or tight-fitting shirt to keep the line and tubes close to the body (Wendel, et al., 2021).
Education of Peers and School Staff
The school nurse may want to discuss with the student and their family about their desire for the student’s peers and school staff to be made aware and educated about the student’s underlying health condition and/or need for a central venous line. Depending on the student and family’s wishes, educating peers may help alleviate endless questions and help teach peers on how to be supportive and inclusive.
Student
Health History Questions: The school nurse may want to ask the student and their parents/guardians the following questions:
- Current health conditions
- Medications
- Allergies
- Previous hospitalizations and surgeries
- Most recent hospitalization
- Location of central venous device
- Exit site of central venous device
- Date of surgical placement
- Device specific information
- Manufacturer name
- Model/Lot number
- Catheter length
- Catheter size (french)
- Number of lumens
- Home health agency
- Insurance coverage
- Health care provider(s) name and contact information
- Preferred hospital, if applicable
Assessment Questions: The school nurse may want to consider asking the student and their parents/guardians the following questions:
- How does this health condition impact the student’s daily life?
- How often does the student miss school due to their health condition(s)?
- Tell me about your friends.
- How often do you spend time with them?
- Has the student shared information about their health condition(s) with their friends/peers?
- Does the student require activity precautions to prevent injury?
- Does the student have specific hydration requirements?
- Does the classroom environment support the student’s needs (i.e., desk/seating options)?
- Does the student and/or their parents/guardian have any concerns related to the student’s health condition?
- Do you feel the student has been sufficiently supported by the school staff in managing their health condition?
- Who has the student been going to when they need help?
- How often does the student have bad feelings about coming to school because they are worried/afraid/embarrassed about something (peers, assignments, teacher)?
- What challenges does the student face in dealing with their health condition?
- Has the student had to change any of their social activities because of their CVL or underlying health condition?
- Has the student ever been picked on or bullied?
- Does the student attend before or after school care?
- Does the student participate in school-sponsored clubs or athletics?
- Would the student benefit from evaluations or assessments in any of the following areas: physical therapy, occupational therapy, speech and language therapy, assistive technology, adapted physical education, functional behavior, psychology, hearing and vision?
- Would the student benefit from additional academic support and/or modified education (i.e., copies of notes, extra time, reduced workload, simplified instructions, alternative formats for presentation of material, 504/IEP)?
- Does the student have an Individualized Health Care Plan (IHCP)?
- Is there a need for a specific plan for this student’s individual needs if there is a crisis in the building?
- If shelter-in-place were required or the school day needed to be unexpectedly extended, what additional supplies, equipment, and health care provider orders would be needed?
- How is the student transported to and from school?
(Clarke, Embury, & Yssel, 2014; Llorens, McKee, & Dempsey, 2020).
Transition Planning:
The school nurse should assess the student’s current and desired level of independence to determine what goals should be established for the student. Additionally, the school nurse should discuss with the student and family what steps have been initiated related to transition planning. The school nurse should consider including goals related to self-management and decision-making skills in the student’s Individualized Health Care Plan (IHCP) (NASN, 2019b) and consider how those goals can be expanded upon each year to support independence, if appropriate.
Transportation:
Given the other health conditions that the student may have they may require special services when being transported to and from school. The school nurse may need to train school bus drivers or assistive personnel on how to respond to an emergency if it were to occur on the school bus.
Communication
It is important for the school nurse to discuss with the student and their family the best way(s) to communicate with them. Does the parents/guardian have a preference (i.e., email, text, telephone call)? Do the parents prefer to have the communications sent to both parents or is there a parent who manages the communication with the school nurse?
The school nurse may want to consider having the parents/guardians complete a Health Insurance Portability and Accountability Act (HIPAA) compliant medical release form to facilitate communication with the student’s health care team. Although HIPAA does not require parental consent to allow the school nurse to discuss the student’s treatment plan, such as medications and nursing procedures, with the student’s health care provider, having a signed consent form would undoubtedly make the process go smoother for all involved parties (U.S. Department of Health and Human Services & U.S. Department of Education, 2008).
FERPA HIPAA Consent Sample (NASN)
Medication
Many children who have gastrostomy tubes will receive their medications via that route. The school nurse should be sure to review the health care provider’s order to confirm all the necessary information is included.
Health Care Provider Order:
For students who require medication administration via g-tube the following information should be included in the health care provider’s order:
- Name of the student
- Date of birth
- Name of medication
- Dose
- Route
- Time of administration
- Reason for administration
- Amount of water flush to be administered pre-medication administration
- Amount of water flush to be administered post-medication administration
- Method(s) to verify placement, if required
- Actions to take if g-tube becomes dislodged
If the medication to be administered via gastrostomy tube is a pill or capsule, the school nurse should check with a pharmacist or review a drug administration reference to confirm the medication can be crushed or the capsule can be opened (Perry, et al., 2021).
Delegation of Medication Administration:
Given that medication administration via a gastrostomy tube is more complex than oral medication administration, the school nurse needs to consider who has the appropriate knowledge, abilities, skills, and willingness to administer the medication. See the Delegation section for more information. The National Association of School Nurses has developed a Medication Administration Delegation Checklist that school nurses may find helpful when making decisions regarding delegating medication administration.
Field Trips
Field trips and other out of school activities can add a layer of complexity to the care of a student with a gastrostomy tube, especially if the student will require an enteral feeding or medication administration while on the field trip. There are several variables that the school nurse will want to consider and plan for, including:
- Who will accompany the student on the field trip to perform necessary procedures or administer medication?
The individual who will be providing the care or performing the procedure must have the knowledge, ability, skills, and willingness to perform the procedure (Erwin, Clark, & Mercer, 2014). - Where will the supplies, enteral feeding, and medications be stored?
It is important to have all needed supplies readily available. Supplies should not be left on the bus but should be with the student at all times. This could require some planning if the enteral formula needs to be refrigerated (Erwin, Clark, & Mercer, 2014). - How will the student’s privacy be protected?
The school nurse should discuss with the student and their family where the procedures will be performed during the field trip and the student and family’s expectations related to privacy. - How will safety and cleanliness be ensured?
In addition to privacy, the school nurse must think through possible scenarios on where the procedure may be performed and what additional precautions and supplies may be needed to ensure safety and cleanliness. - How will the procedure be documented?
Timely documentation is a key component of nursing. The school nurse should consider how procedures and medication administration that occur on a field trip will be documented (Erwin, Clark, & Mercer, 2014; NASN, 2021). - How will the student’s Emergency Action Plan (if applicable) be modified on the field trip?
The school nurse will want to consider any potential emergencies that may arise on the field trip and develop plans on how to address them. The school nurse would want to determine where hospitals are in relation to the field trip route or destination and identify the average Emergency Medical Services (EMS) response time. This information should then be used to make any necessary modifications to the Emergency Action Plan (NASN, 2019a). - Is the field trip occurring out of state or out of the country?
Field trips that occur out of the student’s home state will require some additional planning. If the school nurse will be accompanying the student on the field trip, they will want to determine if the state(s) that will be traveled through or visited are a part of the Nurse Licensure Compact.
If the school nurse will not be accompanying the student but instead will be delegating the procedures, the school nurse will want to review the other state’s nurse practice acts and associated rules and regulations to determine if the procedure can be delegated to a UAP in that state.
For out of the country field trips, the school nurse should discuss with school administration any applicable laws to determine what additional steps may be needed. In addition, the U.S. Embassy can provide information on points of contact for destination countries.
The school will also want to connect with the student’s parents/guardians regarding informing the Transportation Security Administration about the student’s health needs.
(Erwin, Clark, & Mercer, 2014; NASN, 2019a; Wisconsin Department of Public Instruction, 2019)
It is important to note that the Section 504 of the Rehabilitation Act does not allow for a student with a disability to be excluded from a field trip due to their disability.
Documentation
The medical management of a student with a gastrostomy tube in the school setting will require the school nurse to acquire and complete numerous forms of documentation.
Health Care Provider Order:
For students who require tube feedings at school, the following information should be included in the health care provider’s order:
- Student’s name
- Date of birth
- Type of formula
- Volume of formula to be infused
- Frequency of infusion
- Method of infusion (i.e., bolus, intermittent feeding via pump, continuous infusion via pump)
- Rate of infusion (for feedings via pump)
- Reason for infusion
- Method(s) to verify placement, if required
- Residual check
- How residual volume should be returned to the stomach (i.e., gravity, added to volume to be infused, etc.)
- The residual amount that would prohibit feeding at the prescribed time
- Amount of water flush:
- Pre-feeding
- Post-feeding
- Pre-medication administration
- Post-medication administration
- Position of the student during and after feeding
- Venting of g-tube post feeding
- Actions to take if g-tube becomes dislodged
- G-tube site care
For students who require medication administration through a g-tube: See the Medication section for recommendations on information that should be included in the health care provider’s order.
Emergency Action Plan: Students with gastrostomy tubes will require planning related to possible emergencies that may occur at school, including but not limited to, dislodgement of the g-tube or aspiration (Oley Foundation, 2022). The Emergency Action Plan should include:
- Definition of medical emergency for this student.
- Signs of an emergent or worsening condition with steps to take to remediate or when to seek EMS care.
- Specific actions to be taken in the emergency, based on the signs and symptoms present.
- List of individuals to be notified when this emergency occurs.
- Transportation procedures (Missouri Department of Elementary and Secondary Education & Missouri Department of Health and Senior Services, 2014, pp.72, 85).
The school nurse could develop an Emergency Action Plan and incorporate the emergency steps, including the necessary training of school staff, into the Individualized Health Care Plan. If the student has a Section 504 Plan or IEP, these emergency steps and planning should be documented in those plans as well.
Parent/Guardian Authorization: In addition to the health care provider’s order, the school nurse will also need written authorization from the parents/guardians to perform gastrostomy procedures at school. The authorization form can be a separate document that just the parents sign or a document can be developed that combines the health care provider’s order and parent authorization in one form.
Medication Authorization (NASN)
Procedures and Medication Administration: All medication administration, feedings, and gastrostomy tube related procedures will need to be documented, whether they are performed by the school nurse, a UAP, or the student. Many times the medication administration and procedures are documented in the student’s health record. The school nurse will also want to ensure that medications being administered or procedures being performed during field trips, before or after school, and/or during any school-sponsored activities are being documented.
Staff Competency Validation: If the procedures or medication administration is delegated to a UAP the school nurse should document that the UAPs knowledge, abilities, and skills have been assessed. Many times these factors are documented on a skills competency checklist (see Skill Competency Checklists[1] ). There should be a place on the skills competency checklist for the school nurse and UAP to sign to indicate that they feel competent and are willing to perform the procedure. Once the procedure has been delegated the school nurse is responsible for periodic evaluation of the UAP and their competency. The school nurse must determine how often the supervision is needed. After the school nurse has re-evaluated the UAP’s competency, they should document the date of the evaluation (Selekman & Ness, 2019; Shannon & Kubelka, 2013). The school nurse should organize the competency documentation in a way that easily allows them to determine when subsequent evaluation and documentation of competency is needed. For more information on delegation see the Delegation section.
Individualized Health Care Plan (IHCP): IHCPs should outline the plan of care for the student, including but not limited to:
- Actions the school nurse will take to support the student’s educational attainment.
- The education and training that will be provided to school personnel.
- The development of Emergency Action Plans, including steps to be taken in case of an evacuation.
- And the accompanying expected outcomes for each of the nursing interventions (NASN, 2020d).
Prior to completing the IHCP, the school nurse should complete a health history and physical assessment of the student. For more information on health history see the Student section.
Section 504 Plan: Students with gastrostomy tubes may qualify for a Section 504 Plan since their health condition may impact a major life activity (eating). If the student has been identified as qualifying for a 504 Plan, the school nurse may be involved in identifying appropriate accommodations and writing the plan. Once developed, the school nurse will want to frequently review, update, and document in the 504 Plan (NASN, 2020d).
For more information on Section 504 Plans see Legal Issues section
Individualized Education Program (IEP): If a student with a g-tube has an IEP where “related services” include nursing services, the school nurse will want to ensure they are providing and documenting the related services in the student’s education record, whether this is paper or electronic. This documentation is necessary for the school to validate that they are providing the services that the student has been determined to be eligible for under the Individuals with Disabilities Education Act (IDEA) (Galemore & Sheetz, 2015).
Procedures
Link to Just in Time Learning > Digestive resources
Emergency Procedures
Shelter-in-Place and Other Emergency Events:
In addition to an Emergency Care Plan (see Documentation section), the school nurse must also plan for other potential emergencies such as lockdown, extreme weather events, evacuations, and shelter-in-place events. To develop plans to address these possible emergencies the school nurse would want to collaborate with other school staff and administrators. Considering that a student who requires a g-tube may also have physical and cognitive disabilities that could impact their ability to independently respond in an emergency or to follow commands, the school nurse and team will want to incorporate all the student’s individual factors into the planning. The emergency preparedness plan should address the following:
- Location of extra supplies in case of lock-down.
- Provision of supplies that may be needed if there is no access to electricity.
- Access to extra enteral feeding in case of unplanned extended school day or shelter-in-place.
- Health care provider’s orders for enteral feedings that would be necessary if there was an unplanned extended school day or shelter-in-place.
- Additional accommodations that may be required during an emergency (i.e., extra staff to help support the student’s needs).
- Equipment and/or transportation needed to assist with evacuation if the child has limited mobility.
(Center for Inclusive Child Care, 2020; Federal Emergency Management Agency, 2009)
For more information on emergency planning see Missouri School Boards’ Association’s Emergency Planning Guide for Students and Staff with Special and Functional Needs within Schools.
Legal Issues
Section 504 Plan:
Students with a gastrostomy tube may qualify for a Section 504 Plan. Section 504 of the Rehabilitation Act of 1973 as amended through the Americans with Disabilities Amendment Act (ADAA) in 2008 ensures that students who have disabilities have access to a free and appropriate public education (FAPE) (U.S. Department of Education, 2023). FAPE provides a student with a physical or mental impairment that impacts one or more major life activities (including eating) with related services and accommodations in the general education classroom (U.S. Department of Education, 2023; NASN, 2023). If the student does not have a 504 Plan the school nurse should determine if an evaluation is indicated (see Student section for questions to ask student and family to determine if 504 or IEP evaluation is indicated). If it is determined that the student qualifies for a Section 504 Plan, the school nurse may want to consider the appropriateness of the following accommodations:
- Administering the tube feeding where the student is most comfortable (i.e. nurse’s office, lunch room, or classroom)
- Designated individual who is responsible for administering the tube feeding (nurse or UAP)
- Use of specific chairs or positioners during and following tube feeds (for children who need to be in an upright position to manage reflux or other medical issues)
- Monitoring for safety during tube feedings
- Stoma site management by school nurse or UAP, as needed
- Emergency plan should the tube become dislodged at school (Homer, 2020; Lechneer, 2018)
Individualized Education Program (IEP):
In addition to their health condition, a child who requires a g-tube may also have another condition, such as an intellectual disability or significant developmental delay, that qualifies them for an IEP (U.S. Department of Education, 2018). An IEP is developed by a multidisciplinary special education team. The IEP outlines the plans for special education services for the student who has a qualifying disability that interferes with learning. The IEP plan identifies what services and accommodations are needed to support the student’s education needs (NASN, 2020d). Many interventions provided as part of the IEP plan are “related services”, which include school nursing services and school health services (U.S. Department of Education, 2017).
Resources
American College of Surgeons. Feeding Tube Home Skills Program. https://www.facs.org/for-patients/home-skills-for-patients/feeding-tube/
American Society for Parenteral and Enteral Nutrition (ASPEN) https://www.nutritioncare.org/
Avanos Medical. TubeFed.com https://tubefed.com/
Feeding Matters https://www.feedmatters.org/
The Oley Foundation https://oley.org/
References
Abbott Laboratories. (2020). Gravity tube feeding overview.
American Academy of Allergy, Asthma, and Immunology. (2023). SA³MPROTM Establishing a circle of support.
American Nurses Association. (2012). Principles of delegation.
Anderson, C.E. & Herring, R. A. (2024). Pediatric nursing interventions and skills. In Hockenberry, Duffy, & Gibbs (Eds). Wong’s nursing care of infants and children (12th Ed., pp. 669-738).
Applied Medical Technology. (2013). What is a traditional length G-tube?
Avanos Medical. (2018). Percutaneous endoscopic gastrostomy (PEG) tubes.
Boullata, J. I., Carrera, A. L., Harvey, L., Escuro, A. A., Hudson, L., Mays, A., McGinnis, C., Wessel, J. J., Bajpai, S., Beebe, M. L., Kinn, T. J., Klang, M. G., Lord, L., Martin, K., Pompeii-Wolfe, C., Sullivan, J., Wood, A., Malone, A., Guenter, P., & ASPEN Safe Practices for Enteral Nutrition Therapy Task Force, American Society for Parenteral and Enteral Nutrition. (2017). ASPEN safe practices for enteral nutrition therapy [Formula: see text]. JPEN. Journal of parenteral and enteral nutrition, 41(1), 15–103.
Center for Inclusive Child Care. (2020). Tip sheets. Emergency planning for children with disabilities.
Clarke, L.S., Embury, D.C., Yssel, N. (2014). Supporting students with disabilities during school crisis. A teacher’s guide. Teaching Exceptional Children, 46(6), 169-78. doi/10.1177/0040059914534616
Erwin, K., Clark, S., & Mercer, S.E. (2014). Providing health services for children with special health care needs on out-of-state field trips. NASN School Nurse, 29(2), 84-8. doi: 10.1177/1942602X13517005
Farou, N., Lucas, C., & Olympia, R.P. (2021). School nurses on the front lines of healthcare. Children with medical devices-A “bolus” of information about gastrostomy tube malfunctions and infections. NASN School Nurse, 36(3), 144-48.
Federal Emergency Management Agency. (2009). Evacuating the special needs population.
Feeding Tube Awareness Foundation. (2014). What you need to know. A parent’s introduction to tube feeding.
Galemore & Sheetz. (2015). IEP, IHP, and section 504 primer for new school nurses. NASN School Nurse, (Print), 30(2), 85–88. https://doi.org/10.1177/1942602X14565462
Homer, E.M. (2020). Swallowing (dysphagia) and feeding services in the school setting: Things parents should know.
Kennedy Krieger Institute. (n.d.). Enteral feeding tubes.
Kyle, T. & Carman, S. (2021). Essentials of pediatric nursing.
Lechneer, K. (2018). School based accommodations and supports.
Lemanske, R.F., Kakumanu, S., Shanovich, K., Antos, N., Cloutier, M.M., Mazyc,k D., et al. (2016). Creation and implementation of SAMPRO™: A school-based asthma management program. J Allergy Clin Immunol. doi: 10.1016/j.jaci.2016.06.015
Llorens, A., McKee, S., & Dempsey, A.G.). (2020). In A.G. Dempsey (Ed.). Pediatric health conditions in schools. (pp. 26-27). New York, NY: Oxford Press.
Lynn, P. (2019). Administering a tube feeding. In Skill checklists for Taylor’s clinical nursing skills. A nursing process approach. (5th ed.). (pp. 253-255).
Lynn, P. (2019). Confirming placement of a nasogastric tube. In Skill checklists for Taylor’s clinical nursing skills. A nursing process approach. (5th ed.). (pp. 251-252).
McClanahan, R., Shannon, R.A., Kahn, P. (2019). School health office management. In J. Selekman, Shannon, R.A., Yonkaitis, C.F. (Eds.). School nursing, a comprehensive text (3rd ed., pp. 888-908). Philadelphia PA.: F. A. Davis Co.
Medline Plus. (2022). Tube feeding [Image].
Missouri Department of Elementary and Secondary Education & Missouri Department of Health and Senior Services. (2014). Manual for school health programs.
National Association of School Nurses. (2019a). School-sponsored trips -The role of the school nurse (Position Statement). Silver Spring, MD: Author.
National Association of School Nurses. (2019b). Transition planning for students with healthcare needs (Position Statement). Silver Spring, MD: Author.
National Association of School Nurses. (2020a). Emergency medication toolkit.
National Association of School Nurses. (2020b). Fact sheet for school administrators, families, and school personnel. Members of a student’s circle of support.
National Association of School Nurses. (2020c). Fact sheet for school administrators, families, and school personnel. School nurse-led care coordination for students with chronic health conditions.
National Association of School Nurses. (2020d). Understanding student health and education plans.
National Association of School Nurses. (2020e). Use of individualized healthcare plans to support school health services (Position Statement). Silver Spring, MD: Author.
National Association of School Nurses. (2021). Medication administration clinical practice guidelines in the school. Author.
National Association of School Nurses. (2023). IDEIA and Section 504 Teams – The school nurse as an essential team member (Position Statement). Author.
Oley Foundation. (2022). Tube feeding troubleshooting guide.
Perry, A. G., Potter, P.A., Ostendorf, W., & Laplante, N. (2021). Skill 21.2 administering medications through a feeding tube. In Clinical nursing skills and techniques. (10th ed.). (pp. 613-618). St. Louis, MO: Elsevier.
Perry, A. G., Potter, P.A., Ostendorf, W., & Laplante, N. (2021). Skill 32.2 verifying placement of a feeding tube. In Clinical nursing skills and techniques. (10th ed.). (pp. 959-963). St. Louis, MO: Elsevier.
Perry, A. G., Potter, P.A., Ostendorf, W., & Laplante, N. (2021). Skill 32.4 administering enteral nutrition: Nasogastric, nasointestinal, gastrostomy, or jejunostomy tube. In Clinical nursing skills and techniques. (10th ed.). (pp. 965-972). St. Louis, MO: Elsevier.
School Health Associates. (2023). Low profile device with balloons deflated and inflated [photo]. October 25, 2023.
School Health Associates. (2023). Standard length g-tube with bumper and inflated balloon [photo]. October 25, 2023.
Schwartz, L. (2014). Choosing the right tube for you.
Selekman, J. & Ness, M. (2019). Students with chronic conditions. In J. Selekman, R.A. Shannon, C.F. Yonkaitis, (Eds.). School nursing, a comprehensive text (3rd ed., p 493). Philadelphia PA.: F. A. Davis Co.
Shannon, R. A., & Kubelka, S. (2013). Reducing the risks of delegation: use of procedure skills checklists for unlicensed assistive personnel in schools, Part 2. NASN School Nurse (Print), 28(5), 222–226. https://doi.org/10.1177/1942602X13490030
Spratling, R., Chambers, R., Lawrence, P., & Faulkner, M.S. (2021). Best practices with use of feeding tubes for children at home. Pediatric Nursing, 47(1), 7-10.
University of Chicago Medicine. (2021). Possible g-tube problems. Available at: https://www.uchicagomedicine.org/-/media/pdfs/comer-pdfs/conditions-and-services/general-surgery/g-tube/g-tube-problems.pdf
U.S. Department of Education. (2017, May 2). Sec. 300.34 related services. Available at: https://sites.ed.gov/idea/regs/b/a/300.34
U.S. Department of Education. (2018, May 25). Sec. 300.8 Child with a disability.
U.S. Department of Education. (2023). Frequently asked questions about Section 504 and the education of children with disabilities.
U.S. Department of Health and Human Services & U.S. Department of Education. (2008). Joint guidance on the application of the Family Educational Rights and Privacy Act (FERPA) the Health Insurance Portability and Accountability Act of 1996 (HIPAA) to student health records.
Wisconsin Department of Public Instruction. (2019). Meeting student health needs while on field trips. Tool kit for Wisconsin schools.
Reviewers
Renee Falkner, BSN, RN
School Nurse Supervision Specialist | Therapylog
Katherine Park, DNP, RN, NCSN
Nationally Certified School Nurse, Pierremont Elementary
Adjunct Professor, Maryville University School of Nursing
Last updated 4/18/2025
More Information
