Cystic Fibrosis, Endocrine
This resource provides current and comprehensive health care information for school health nurses. Related procedures, instructional videos and downloadable skills checklists can be searched by selecting the [More Information] button at the bottom of this web page.
Overview
Cystic Fibrosis (CF) is an inherited chronic health condition characterized by exocrine (or mucus-producing) gland dysfunction. CF is characterized by:
- Increased viscosity of mucous gland secretions
- Elevation of sweat electrolytes
- Increase in several organic and enzymatic constituents of saliva
- Abnormalities in autonomic nervous system function
“The faulty gene that causes cystic fibrosis disrupts the normal flow of salt and water in and out of the lungs and other organs. This salt imbalance results in thick, sticky mucus that builds up in the lungs, allowing germs to thrive and multiply” (Cystic Fibrosis Foundation, n.d.h.). Almost all children with CF will have pulmonary complications but the onset and severity will vary. Complications arise due to stagnation of mucous in the airways and bacterial colonization which leads to destruction of the lung tissue.
Symptoms associated with CF depend on which organs are affected and how severe the condition is. The most common symptoms associated with CF affect the lungs and include a chronic cough and wheezing. The student’s cough may be disruptive to the class and the teacher may suggest that the student leave the classroom or go get some water. It is important that the school nurse advocates for the student and talks with the teacher(s) to educate them about the student’s cough. The student should be permitted to leave the classroom, if that makes them feel more comfortable but should not feel as though they are required to. Additionally, students with CF should not be given medications to suppress their cough or dry up their secretions, as these medications are counterproductive to having the student thinning the mucus and coughing it out (Barrett & Murphy Moore, 2019). Some additional symptoms that may affect the school-aged child include:
- Clubbing of fingers and toes due to less oxygen getting to the hands and feet
- Delayed puberty
- Fertility problems, especially for males
- Fever, which may include night sweats
- Gastrointestinal symptoms such as severe belly pain, chronic (long-term) diarrhea, or constipation
- Infections of sinuses and lungs
- Low body mass index (BMI) or being underweight
- Muscle and joint pain
- Pancreatitis
- Salty skin and extra-salty sweat
- Slow growth and shorter height
(National Heart, Lung, and Blood Institute, 2023)
Image: Organs Affected by Cystic Fibrosis
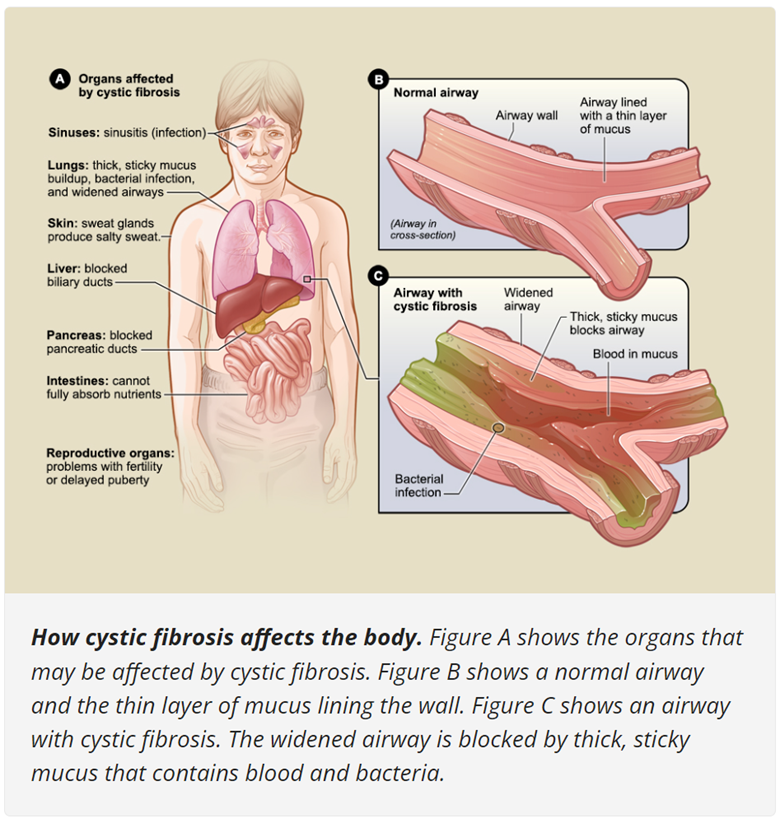
Source: National Heart, Lung, and Blood Institute, 2023
Infections:
Infections in people with CF pose a serious problem and can lead to worsening lung disease or death. The sticky mucus that builds up in the student’s lungs, allows germs to thrive and multiply. People with an otherwise healthy immune systems may be able to fight off these infections but people with CF are not. The most common respiratory pathogens include:
- Methicillin‐resistant Staphylococcus aureus (MRSA):
MRSA is strains of Staphylococcus aureus that are resistant to commonly used antibiotics. MRSA can be spread from one person to another through casual contact, like shaking hands, or by touching objects that have the bacteria on them. - Pseudomonas aeruginosa (P. aeruginosa):
Pseudomonas is a common bacteria that come in thousands of different strains and is found in many different environments. Some strains have become resistant to multiple antibiotics and can be very hard to treat. Medical data show that people with CF may pick up these more difficult‐to‐treat strains of the bacteria from each other. - Aspergillus:
Aspergillus is a common mold (a type of fungus) found indoors and outside. It causes a disease called Aspergillosis, which usually only develops in people with weakened immunity or lung disease. - Nontuberculous mycobacteria (NTM):
This group of bacteria lives in soil, swamps, and water sources. NTM can survive many disinfectants and severe environmental conditions. The bacteria have been found in growing numbers of people with CF (Cystic Fibrosis Foundation, n.d.h.). - Burkholderia cepacia complex:
The Burkholderia cepacia complex (B. cepacia) consists of different species of bacteria that are found in the natural environment. Some of these species pose serious risks to the health of a person with cystic fibrosis. Burkholderia bacteria are often resistant to many antibiotics, which makes them difficult to treat once they infect the lungs. However, some species may be successfully treated with combinations of antibiotics. Basic infection prevention and control practices reduce the risk of getting or spreading B. cepacia. These bacteria pose very little medical risk to healthy people. Students with cystic fibrosis could be impacted differently by B. cepacia complex species. Some students with cystic fibrosis B. cepacia complex species can lead to a rapid decline in lung function and health (Cystic Fibrosis Foundation, n.d.b.).
It is not known how students with cystic fibrosis become infected with B. cepacia complex. Students with cystic fibrosis can get B. cepacia from others who are infected with these bacteria. The germs spread either by direct contact (i.e. kissing) or indirectly from touching objects with the germs. This is known as cross-infection and can happen in social settings like events, gatherings or meetings (Cystic Fibrosis Foundation, n.d.b.).
Cystic Fibrosis-Related Diabetes (CFRD):
CFRD shares features to both type 1 and type 2 diabetes. In CFRD the pancreas does not make enough insulin (type 1) due to scarring on the pancreas and some students can develop insulin resistance (type 2) especially when they are ill. The goal for students with CFRD is to maintain their blood glucose at normal or near-normal levels and to maintain good nutrition. Depending on the severity of the disease, some students may require insulin administration, either through shots or an insulin pump. Some students may also have a continuous glucose monitor (Cystic Fibrosis Foundation. n.d.d.; Cystic Fibrosis Foundation, 2023).
The Cystic Fibrosis Foundation has developed a Managing Cystic Fibrosis-Related Diabetes–An Instruction Guide for Patients and Families.
Treatment for CF:
There are numerous treatments for CF that a student may be prescribed, including medications, enzymes, and Airway Clearance Therapy. See the Medications and Procedure sections for more information.
Delegation
If the student receives ACTs at school, the school nurse may choose to delegate to a unlicensed assistive personnel (UAP). If the physical therapist is involved in training of the UAP, it may be the PT who delegates the procedure.
Questions to Ask to Inform Safe Delegation: The delegation questions below are based on the American Nurses Association’s Decision Tree for Delegation by Registered Nurses (ANA, 2012).
- Has the school nurse performed an initial assessment of the student to determine their needs? The school nurse should not delegate the procedure to a UAP until they have completed the initial assessment.
- Does school district policy, the school nurse’s job description, and the UAP’s job description allow procedures related to ACTs to be delegated? Although the Missouri Nurse Practice Act allows for registered nurses to delegate ACT procedures, the district may have policies that prohibit or limit the school nurse’s ability to delegate. Additionally, the school nurse’s & UAP’s job descriptions may restrict delegation as well.
- Is the school nurse competent to perform this procedure or does the school nurse need to acquire some knowledge or skills to be competent in this procedure? If the school nurse is not competent or does not feel comfortable performing this procedure, they should not delegate this procedure to a UAP. The school nurse must first acquire the necessary knowledge and skill to perform this procedure competently before they can delegate it to someone else.
- Is the student’s condition stable? How predictable are the outcomes of the procedure? A school nurse should not delegate the ACT procedures to a UAP if the outcomes are not predictable. The school nurse should perform the procedures until the student’s condition has stabilized.
- Does the procedure require an initial or ongoing assessment to be performed during the procedure? If an initial or ongoing assessment is required for the procedure to be performed, the procedure should not be delegated.
- Does the UAP have the appropriate knowledge, skills, abilities, and willingness to perform the procedure? All these factors need to be considered. Although a UAP may be competent to perform the procedure they may not be willing to do so and in that situation another UAP should be identified and trained. The registered nurse must retain responsibility for the procedure until training is complete.
- Is there a procedure and/or protocol in place for this procedure? A delegated nursing procedure must have an established sequence of steps that the UAP can follow. These steps should have a predictable outcome. The steps should be outlined in a written procedure or protocol. If the written procedure/protocol has not been developed, the school nurse should retain responsibility for the procedure until the procedure/protocol is in place.
- Is the school nurse able to provide supervision to the UAP (direct or indirect depending on the situation)? If the school nurse is not able to provide supervision, then the procedure should not be delegated. The school nurse will need to assess the situation to determine if direct or indirect supervision is required. The school nurse may also need to reassess the situation if the environment changes, for example, if the procedure is going to be performed during a time that the school nurse is not contracted to provide nursing services (i.e., over the weekend, during the summer, or if the school nurse is part-time).
- Is the student ready to assume some responsibility for the procedure? The school nurse should resume responsibility for the procedure since the school nurse is the only one who can initiate teaching. The school nurse would also want to observe the student performing the procedure to ensure that the student is competent. Once the school nurse has determined that the student is competent and can safely perform the procedure independently, they can delegate the supervision of the student to a UAP. If at a future date the school nurse is needed to teach the student additional skills, the school nurse would again need to resume responsibility for the procedure until the time in which the school nurse determined the student to be competent.
The Decision to Delegate:
There may be times when the school nurse and school administrator have conflicting opinions on the delegation of a procedure to a UAP. The school nurse may feel that delegation is not appropriate or the administrator may want the school nurse to delegate a procedure to an UAP that the school nurse feels is not competent. In these situations the school nurse may need to educate the administrator that the school nurse has a professional and legal responsibility to determine if delegation of a nursing procedure is appropriate and safe (ANA, 2012).
A resource developed by the National Association of School Nurses entitled, Fact Sheet for School Administrators, Families, and School Personnel: Nursing Delegation Requires the School Nurse may assist the school nurse in communicating with the school administration.
Learn more at Navigating Delegation in the School Setting (PDF)
School Environment
Physical Environment:
When There is More Than One Student with Cystic Fibrosis (CF):
Because everyone with CF carries different germs in their lungs there is a risk they can pass these on to other people with CF, this is called cross-contamination. It is recommended that two people with CF not be within 6 feet of each other. In a school setting, Due to these requirements, considerable planning needs to occur when there will be more than one student with cystic fibrosis in the same school at the same time. The following recommendations from the Cystic Fibrosis Foundation (n.d.f.) should be followed:
- Minimize Time Spent in the Same Place
- Limit the time that two or more people with CF can spend in one place. A minimum 6-foot distance should be maintained at all times.
- Place people with CF in separate classrooms whenever possible.
- If the students must be in the same classroom, but at different times, make sure the students are assigned separate desks or workstations as far away as possible (a minimum of 6 feet) from the assigned location of other student(s) with CF.
- Assign separate bathrooms and drinking fountains for each student and staff member who has CF.
- The student with CF should use a water bottle if possible since drinking fountains often contain bacteria that is harmful to those with CF (OSF Healthcare, 2024).
- Schedule the students with CF to be in other common gathering areas, such as the gym, at different times.
- Assign lunch tables, lockers, etc. for all students with CF to be as far away as possible from the assigned locations of other students with CF.
- Assign different locations for people with CF to go for their medications, or have the school nurse visit each student in their separate classrooms to administer the medications.
- Assign different places for each person with CF to go if he or she becomes ill while in school.
- For example, one student can go to the health office, another to the principal’s office and a third to the counselor’s office.
- If a student with CF is ill or needs to go to another room or office to get medications, the staff in that office should be notified prior to sending the student to the office to ensure that another person with CF is not present.
Even when there are not two people with CF in the school, the following infection control guidelines should be implemented:
- Everyone Should Wash Their Hands
- Encourage everyone to wash or clean their hands. Germs can spread when people touch something with germs already on it, like a doorknob or desk, and then touch their eyes, nose or mouth.
- Make alcohol-based hand gel and or soap and water readily available for all students and staff to use in the classrooms.
- Everyone should clean their hands after coughing, sneezing or blowing their nose and after using common equipment like pencil sharpeners and lab equipment.
- This is especially important during the cold and flu season.
- This is especially important during the cold and flu season.
- Everyone Should Cover Their Cough
- Encourage everyone to cover their cough. Germs can remain in the air on tiny droplets — ready to be breathed in. They can also remain on surfaces long after a person has coughed or sneezed on or near them.
- Make tissues readily available and encourage people to cough or sneeze into a tissue and throw it away immediately before washing or cleaning hands.
- If a tissue is not available, encourage everyone to cough or sneeze into their inner elbow.
- Everyone Should Get Vaccinated
- Encourage everyone to get vaccinated. Vaccinations help the body protect itself from germs, like the flu virus, which are especially dangerous for people with CF.
See the Cystic Fibrosis Foundation’s article How Can You Reduce the Risk of Cross-infection?
Physical Education and Recess:
The school nurse should review the health care provider’s order to see if there are any activity restrictions or precautions during physical education class or at recess. The student may need to drink more water or sports drink during times of increased physical activity, especially when there is increased temperature. The school nurse should review the student’s health care provider’s order and communicate with the student and their parents/guardians about any accommodations that are needed. Additionally, the student may have restrictions regarding going outside if the temperature is above or below a certain temperature.
Education of Peers and School Staff:
The school nurse should discuss with the student and their family about the student’s desire for the student’s peers and school staff to be made aware and educated about the student’s CF. Depending on the student and family’s wishes, educating peers may help alleviate endless questions and help teach peers on how to be supportive and inclusive. At a minimum, the student’s educational team should be educated about what signs and symptoms should be reported to the school nurse and parents/guardians and how infection control practices should be implemented in the classroom and school. See Overview section for more information.
Students
An important first step when caring for a student who is diagnosed with a CF would be to complete a health history and physical assessment, preferably with the student and their parents present.
Health History Questions:
- Medical conditions
- Medications
- Allergies
- Previous hospitalizations
- Does the student require meal modifications or substitutions?
- What ACTs does the student utilize?
- Does the student require ACT at school?
- Insurance coverage
- Health care provider(s) name and contact information
- Preferred hospital, if applicable
Assessment Questions: The school nurse may want to consider asking the student and their parents/guardians the following additional questions:
- How does this health condition impact the student’s daily life?
- How often does the student miss school due to their health condition(s)?
- Tell me about your friends.
- How often do you spend time with them?
- Has the student shared information about their health condition(s) with their friends/peers?
- Does the student have specific hydration requirements?
- Does the student have activity restrictions?
- Does the classroom environment support the student’s needs?
- Does the student wear a medical alert bracelet, necklace, watchband?
- Has the student shared information about their diagnosis of CF with their peers?
- Does the student or parents have any concerns about the student’s health condition?
- What challenges does the student face in managing their health condition?
- Do you feel the student has been sufficiently supported by school staff in managing their health condition?
- Who has the student been going to when they need help?
- How often does the student have bad feelings about coming to school because they are worried/afraid/embarrassed about something (peers, assignments, teacher)?
- What challenges does the student face in dealing with their health condition?
- Has the student had to change any of their social activities because of their CF?
- Has the student ever been picked on or bullied?
- Does the student have a 504 Plan or Individualized Education Program (IEP)?
- Would the student benefit from evaluations or assessments in any of the following areas: physical therapy, occupational therapy, speech and language therapy, assistive technology, adapted physical education, functional behavior, psychology, hearing and vision?
- Would the student benefit from additional academic support and/or modified education (i.e.., copies of notes, extra time, reduced workload, simplified instructions, alternative formats for presentation of material, 504/IEP)?
- Does the student have an Individualized Health Care Plan (IHCP)?
- Is there a need for a specific plan for this student’s individual needs if there is a crisis in the building?
- How is the student transported to and from school?
- Does the student attend before or after school care?
- Does the student participate in school-sponsored clubs or athletics?
(Clarke, Embury, & Yssel, 2014; Llorens, McKee, & Dempsey, 2020).
Transition Planning:
The school nurse should assess the student’s current and desired level of independence to determine what goals should be established for the student. Additionally, the school nurse should discuss with the student and family what steps have been initiated related to transition planning. The school nurse should consider including goals related to self-management and decision-making skills in the student’s Individualized Health Care Plan (IHCP) (NASN, 2019) and consider how those goals can be expanded upon each year to support independence, if appropriate.
Communication
The school nurse should discuss with the student and their family the best way(s) to communicate with them. Does the parents/guardian have a preference (i.e., email, text, telephone call)? Do the parents prefer to have the communications sent to both parents or is there a parent who manages the communication with the school nurse?
The school nurse may want to consider having the parents/guardians complete a Health Insurance Portability and Accountability Act (HIPAA) compliant medical release form to facilitate communication with the student’s health care team. Although HIPAA does not require parental consent to allow the school nurse to discuss the student’s treatment plan, such as medications and nursing procedures, with the student’s health care provider, having a signed consent form would undoubtedly make the process go smoother for all involved parties (U.S. Department of Health and Human Services & U.S. Department of Education, 2008).
Medications
There are a number of medications that are used to treat cystic fibrosis that may maintain and improve lung function, fight infections, clear mucus and help breathing, or try to improve how well someone’s CFTR protein works. These medications include:
- Antibiotics to treat lung infections
- Anti-inflammatory medicines since inflammation causes many of the changes associated with cystic fibrosis
- Bronchodilators relax and open airways
- CFTR modulators improve how a faulty CFTR protein works. They help with lung function and can help prevent lung problems or other complications.
- Mucus thinners to make it easier to clear the mucus from the airway
(National Heart, Lung, and Blood Institute, 2023)
Enzyme Replacement: Students with CF will also have pancreatic enzyme replacement therapies. These therapies help the body absorb food and necessary nutrients. The student will need to take these enzymes at school since they are required before every meal or snack. If it is appropriate for the student to self-carry and self-administer their enzyme replacements they should be permitted to do so to avoid having to come to the health room or nurse’s office (Cystic Fibrosis Foundation, n.d.c.). The enzyme capsules must not be crushed or chewed. The enzyme capsule may be opened and then sprinkled on a small amount of an acidic food, such as applesauce, if swallowing the pill is difficult. If the enzymes are opened and sprinkled on the food, the food should be eaten immediately rather than prepared in advance (Mennitt, 2012).
Some foods and drinks do not require enzymes because they contain only simple carbohydrates that are digested and absorbed easily such as:
- Fruits
- Juice, juice drinks
- Soft drinks, sports drinks
- Infant rehydrating formulas (like Pedialyte®)
- Tea, coffee (without cream)
- Hard candy (like lollipops)
- Fruit snacks
- Jellybeans
- Gum
- Popsicles, freezer pops, flavored ice
Some young children still need to take enzymes when eating these foods so they stay in the habit of always taking enzymes with food. If they learn that certain foods don’t require enzymes, they may only want to eat those foods (Cystic Fibrosis Foundation, n.d.e.). The school nurse should collaborate with the health care provider and parent/guardian to establish a plan and ensure the necessary orders are in place if the student is take the enzymes when eating these types of foods.
The Cystic Fibrosis Foundation has more information on enzymes.
Insulin: If a student has developed Cystic Fibrosis-Related Diabetes (CFRD) they may be prescribed insulin. For more information on the management of diabetes, including insulin administration, see the Diabetes page.
Health Care Provider Order:
The following information should be included in the health care provider’s order for any medications the student is to receive at school:
- Name of the student
- Date of birth
- Name of medication
- Dose
- Route
- Time of administration
- Reason for administration
For more information on insulin see the Diabetes page.
For more information on the medications used to treat CF see the Overview section.
Field Trips
Depending on the student’s level of severity field trips and other out of school activities could add a layer of complexity to the care of a student with a CF. There are several variables that the school nurse will want to consider and plan for, including:
- Who will accompany the student on the field trip to perform necessary procedures or administer medication?
- The individual who will be providing the care or performing the procedure must have the knowledge, ability, skills, and willingness to perform the procedure (Erwin, Clark, & Mercer, 2014).
- Where will any necessary supplies and medications be stored?
- It is important to have all needed supplies readily available. Supplies should not be left on the bus but should be with the student at all times.
- How will the student’s privacy be protected?
- The school nurse should discuss with the student and their family where the procedures will be performed during the field trip and the student and family’s expectations related to privacy.
- What additional infection control measures need to be considered?
- How will the procedure be documented?
- Timely documentation is a key component of nursing. The school nurse should consider how procedures and medication administration that occur on a field trip will be documented (Erwin, Clark, & Mercer, 2014).
- How will the student’s Emergency Action Plan (if applicable) be modified on the field trip?
- The school nurse will want to consider any potential emergencies that may arise on the field trip and develop plans on how to address them. The school nurse would want to determine where hospitals are in relation to the field trip route or destination and identify the average Emergency Medical Services (EMS) response time. This information should then be used to make any necessary modifications to the Emergency Action Plan (NASN, 2019).
- Will the length of the field trip require additional orders from the student’s health care provider?
- If the student will require procedures or medication administration that falls outside of the normal school day an additional order from the health care provider may be necessary to cover these additional times.
- Is the field trip occurring out of state or out of the country?
- Field trips that occur out of the student’s home state will require some additional planning. If the school nurse will be accompanying the student on the field trip, they will want to determine if the state(s) that will be traveled through or visited are a part of the Nurse Licensure Compact. If the school nurse will not be accompanying the student but instead will be delegating the procedures, the school nurse will want to review the other state’s nurse practice acts and associated rules and regulations to determine if the procedure can be delegated to a UAP in that state. For out of the country field trips, the school nurse should discuss with school administration any applicable laws to determine what additional steps may be needed. In addition, the U.S. Embassy can provide information on points of contact for destination countries. The school will also want to connect with the student’s parents/guardians regarding informing the Transportation Security Administration about the student’s health needs.
(Erwin, Clark, & Mercer, 2014; NASN, 2019; Wisconsin Department of Public Instruction, 2019)
It is important to note that the Section 504 of the Rehabilitation Act does not allow for a student with a disability to be excluded from a field trip due to their disability.
NASN Resource: Field Trip Preparation Checklist
Documentation
The medical management of a student with CF in the school setting will require the school nurse to acquire and complete numerous forms of documentation.
Health Care Provider Order for Medication: The school nurse will need a health care provider’s order for the medication administration. See the Medication section for more information.
Health Care Provider Order for ACT: Many times the student’s ACTs are performed at home but if the student is to receive ACT at school, the school nurse will want to receive an order from a health care provider.
Parent/Guardian Authorization: In addition to the health care provider’s order, the school nurse will also need written authorization from the parents/guardians to administer medications and perform CF related procedures at school. The authorization form can be a separate document that just the parents sign or a document can be developed that combines the health care provider’s order and parent authorization in one form.
Self-Possession and Administration: When determining if a student is capable of carrying and self-administering their medications the school nurse will want to meet with the student and assess their knowledge, ability, and skills to ensure that it is appropriate for them to self-possess and self-administer their medications. Upon completing this assessment the school nurse will want to document their assessment in the student’s health record. The school nurse should also document that the student’s parent/guardian and health care provider agree with the plan of care for the student to self-carry and self-administer their medication. If the student will be self-administering their medication, the school nurse should review their district policy to determine what documentation is required in the student’s health care record.
The National Association of School Nurses has developed a Contract for Student Self-Carry and Self-Administration of Medication that could be used to document the school nurse’s assessment and planning with the student.
Procedures and Medication Administration: All medication administration and CF procedures will need to be documented, whether they are performed by the school nurse, a UAP, or the student. Many times the medication administration and procedures are documented in the student’s health record. The school nurse will also want to ensure that medications being administered or procedures being performed during field trips, before or after school, and/or during any school-sponsored activities are being documented.
Staff Competency Validation: If the procedures or medication administration is delegated to a UAP the school nurse should document that the UAPs knowledge, abilities, and skills have been assessed. Many times these factors are documented on a skills competency checklist. There should be a place on the skills competency checklist for the school nurse and UAP to sign to indicate that they feel competent and are willing to perform the procedure. Once the procedure has been delegated the school nurse is responsible for periodic evaluation of the UAP and their competency. The school nurse must determine how often the supervision is needed. After the school nurse has re-evaluated the UAP’s competency, they should document the date of the evaluation (Selekman & Ness, 2019; Shannon & Kubelka, 2013). The school nurse should organize the competency documentation in a way that easily allows them to determine when subsequent evaluation and documentation of competency is needed. For more information on delegation see the Delegation section.
Individualized Health Care Plan (IHCP): IHCPs should outline the plan of care for the student and include:
- Actions the school nurse will take to support the student’s educational attainment
- The education and training that will be provided to school personnel
- The development of Emergency Action Plans, including steps to be taken in case of an evacuation
- And the accompanying expected outcomes for each of the nursing interventions (NASN, 2020).
The school nurse may also want to consider including the following goals in the student’s IHCP.
The student will:
- Maintain optimal respiratory function and airway clearance by:
- Keep their lungs functioning as well as possible
- Taking their medications
- Avoiding friends when they are ill
- Performing their ACT as recommended
- Avoiding high risk behaviors such as smoking and vaping
- Maintain adequate growth and weight gain pattern
- Demonstrate improved physical activity tolerance in the school setting
Students will:
- Comply with infection control measures
(Barrett & Murphy Moore, 2019, p.545)
Prior to completing the IHCP, the school nurse should complete a health history and physical assessment of the student. For more information on health history see the Student section.
IHCP Templates are available from :
- Cystic Fibrosis Trust from the United Kingdom: https://www.cysticfibrosis.org.uk/sites/default/files/2020-11/Schools%20Individual%20Healthcare%20Plan.pdf
- CF Smart Cystic Fibrosis Education Program: https://cfcccysticfibrosiscc.blob.core.windows.net/assets/contentpage_htmlcontent/3Blank-CF-Health-support-plan-Primary.pdf
Emergency Action Plan: Depending on the severity of the student’s CF and whether or not the student has additional health conditions (diabetes, presence of a gastrostomy tube, and/or central venous access device) an Emergency Action Plan may be necessary. The Emergency Action Plan should address what constitutes an emergency for the individual student (such as respiratory distress), what symptoms will be present if the student is experiencing an emergency, and what steps to take in response to the symptoms.
An Emergency Action Plan template can be found in Missouri Department of Health and Senior Services’ SN CHAT School Nurse Chronic Health Assessment Tool.
Section 504 Plan: Students with CF may qualify for a Section 504 Plan since their health condition may impact a major life activity (breathing). If the student has been identified as qualifying for a 504 Plan, the school nurse may be involved in identifying appropriate accommodations and writing the plan. Once developed, the school nurse will want to frequently review, update, and document in the 504 Plan (NASN, 2020).
For more information on Section 504 Plans see Legal Issues section.
Procedure
Airway Clearance Therapy: Students with CF need to perform “airway clearance therapy” (ACT). ACTs are performed to assist the student in loosening and moving the thick, sticky secretions from the student’s lungs and airway and would be ordered by the health care provider. The school physical therapist (PT) may also be involved in assisting the student with the ACTs.
A short video by the Cystic Fibrosis Foundation provides more information on Airway Clearance Therapies.
All ACTs include huffing. The procedure for huffing includes the Huff Coughing Technique. Procedure for Huff Coughing Technique:
- Having the student sit up straight with their chin tilted slightly up and mouth open.
- Have the student take a slow deep breath to fill their lungs about three quarters full.
- Have the student hold their breath for two or three seconds.
- Have the student exhale forcefully, but slowly, in a continuous exhalation to move mucus from the smaller to the larger airways.
- Have the student repeat this maneuver two more times and then follow with one strong cough to clear mucus from the larger airways.
- Have the student do a cycle of four to five huff coughs as part of their airway clearance.
(Cystic Fibrosis Foundation, n.d.c.).
All ACTs are designed to make it easier for the student to remove the mucus from their lungs and airways. Some additional ACTs are linked below and include:
- Active cycle of breathing:
- A Technique designed to get air behind the mucus making it easier to cough up.
- Autogenic drainage:
- Uses controlled breathing in three phases.
- Chest physical therapy:
- Also known as postural drainage and percussion is when another person uses cupped hands and percussion to loosen mucus from the student’s airways.
- High frequency chest wall oscillation vest:
- A vest that the student wears compresses the chest in and out to create airflow.
- Positive expiratory device:
- Uses resistance to open the airways and get air behind the mucus.
- Airway oscillating device:
- Resistance forces airways to open and vibrations from the device shake the mucus.
(Cystic Fibrosis Foundation, n.d.a.).
The Cystic Fibrosis Foundation has developed the CF Airway Clearance Therapies Clinical Care Guidelines.
Most times a student’s ACTs are performed at home but some students with cystic fibrosis may have a health care provider’s order to have an ACT performed at school. As these treatments are unique to the student, the school nurse will want to meet with the student’s parents/guardians to receive student-specific information about the procedure. If the school nurse requires education and training regarding how to perform the procedure, they should collaborate with the student’s health care team.
Emergency Preparedness
Shelter-in-Place and Other Emergency Events:
In addition to an Emergency Care Plan (see Documentation section), the school nurse must also plan for other potential emergencies such as lockdown, extreme weather events, evacuations, and shelter-in-place events. To develop plans to address these possible emergencies the school nurse would want to collaborate with other school staff and administrators. The emergency preparedness plan should address the following:
- Location of extra supplies in case of lock-down.
- Provision of supplies that may be needed if there is no access to electricity.
- Health care provider’s orders for medications or procedures that would be necessary if there was an unplanned extended school day or shelter-in-place.
- Additional accommodations that may be required during an emergency (i.e., extra staff to help support the student’s needs).
(Center for Inclusive Child Care, 2020; Federal Emergency Management Agency, 2009)
For more information on emergency planning see Missouri School Boards’ Association’s Emergency Planning Guide for Students and Staff with Special and Functional Needs within Schools.
Legal Issues
Students with CF may qualify for a Section 504 Plan. Section 504 of the Rehabilitation Act of 1973 as amended through the Americans with Disabilities Amendment Act (ADAA) in 2008 ensures that students who have disabilities have access to a free and appropriate public education (FAPE) (U.S. Department of Education, 2023). FAPE provides a student with a physical or mental impairment that impacts one or more major life activities (including breathing) with related services and accommodations in the general education classroom (U.S. Department of Education, 2023; NASN, 2023). If the student does not have a 504 Plan the school nurse should determine if an evaluation is indicated (see Students section for questions to ask student and family to determine if 504 or IEP evaluation is indicated). If it is determined that the student qualifies for a Section 504 Plan, the school nurse may want to consider the appropriateness of the following accommodations:
- Allow the student to use the restroom whenever it is needed (digestive problems from CF can cause diarrhea and flatulence)
- Have access to a private bathroom
- Allow the student to take oral or inhaled medication at school
- Allow the student to eat or drink in class, as needed
- Allow the student to cough frequently to clear mucus from the lungs (CF is not contagious)
- Allow the student to be tired in class due to early-morning breathing therapy or staying awake from coughing at night (Nemours Children’s Health, 2018)
- Allow the student to leave class early or have additional time during the school day to take medication
- Adjust school rules to allow the child to take their own medication, like pancreatic enzymes, if appropriate
- Have a plan to get homework or a tutor when the student is ill, including in the hospital
- Give audio or video recordings of missed classes
- Adjust or waive attendance rules
- Allow the student to carry water with them and have unlimited access to water from a faucet
- Develop an Emergency Action Plan
- School notifies parent of increase of illnesses such as RSV, Flu, whooping cough, or COVID-19
- Sanitize high-touch areas, such as door knobs and shared desks
- Student would not be required to complete a test upon return from an absence
- Student would receive extended time on assignments and assessments (this can be helpful during standardized tests if the child needs restroom breaks or a snack) (Cystic Fibrosis Foundation, n.d.c.)
- Allow the student to drink sports drinks with added carbohydrates and salt
- Encourage the student to avoid drinks with caffeine, which can increase fluid loss.
- Allow the student to carry snacks
- Those with CF have high calorie needs and should eat three meals and three snacks daily
- Allow the student to stay indoors if it is colder than 32 degrees Fahrenheit
- Cold weather can make it difficult for those with CF to breathe
- If necessary, determine a plan for mucus clearance during physical activity (OSF HealthCare, 2024)
- Allow the student to move away from classmates who are sick
- Provide an air-conditioned classroom
- Modifications to physical education activities, as needed
- Accommodations related to Cystic Fibrosis-Related Diabetes (Cystic Fibrosis Research Inc., 2015).
- For example of accommodations, see the Diabetes page
Resources
Cystic Fibrosis Foundation: https://www.cff.org/
A teacher’s guide to Cystic Fibrosis: https://www.cff.org/intro-cf/teachers-guide-cystic-fibrosis
Cystic fibrosis fact sheet for schools: https://kidshealth.org/en/parents/cf-factsheet.html
References
American Nurses Association. (2012). Principles of delegation.
Barrett & Murphy Moore, C. (2019). Students with chronic respiratory conditions: Asthma and cystic fibrosis. In J. Selekman, R.A. Shannon, C.F. Yonkaitis, (Eds.). School nursing, a comprehensive text (3rd ed., pp. 523-548). Philadelphia PA.: F. A. Davis Co.
Center for Inclusive Child Care. (2020). Tip sheets. Emergency planning for children with disabilities.
Clarke, L.S., Embury, D.C., and Yssel, N. (2014). Supporting students with disabilities during school crisis. A teacher’s guide. Teaching Exceptional Children, 46(6), 169-78. doi/10.1177/0040059914534616
Cystic Fibrosis Foundation. (n.d.a). Airway clearance techniques .
Cystic Fibrosis Foundation. (n.d.b.). Burkholderia Cepacia Complex (B. Cepacia).
Cystic Fibrosis Foundation. (n.d.c.). Coughing and huffing.
Cystic Fibrosis Foundation. (n.d.d.). Cystic-fibrosis related diabetes.
Cystic Fibrosis Foundation. (n.d.e.). Enzymes.
Cystic Fibrosis Foundation. (n.d.f.). Individualized education programs (IEPs) and 504 plans.
Cystic Fibrosis Foundation. (n.d.g.). When there’s more than one person with CF at school.
Cystic Fibrosis Foundation. (n.d.h.). Why are some germs particularly dangerous for people with CF?
Cystic Fibrosis Foundation. (2023). Managing cystic fibrosis-related diabetes (CFRD). An instruction guide for parents and families. 7th edition.
Cystic Fibrosis Research, Inc. (2015). Cystic fibrosis in the classroom.
Erwin, K., Clark, S., & Mercer, S.E. (2014). Providing health services for children with special health care needs on out-of-state field trips. NASN School Nurse, 29(2), 84-8.
Federal Emergency Management Agency. (2009). Evacuating the special needs population.
Galemore & Sheetz. (2015). IEP, IHP, and section 504 primer for new school nurses. NASN School Nurse, (Print), 30(2), 85–88.
Llorens, A., McKee, S., & Dempsey, A.G. (2020). In A.G. Dempsey (Ed.). Pediatric health conditions in schools. (pp. 26-27). New York, NY: Oxford Press.
Mennitt D. (2012). What is the current FDA-approved therapy to treat pancreatic insufficiency for children with cystic fibrosis?. NASN School Nurse (Print), 27(2), 67–68.
National Association of School Nurses. (2019). School-sponsored trips -The role of the school nurse (Position Statement). Silver Spring, MD: Author.
National Association of School Nurses. (2020). Understanding student health and education plans.
National Association of School Nurses. (2023). IDEIA and Section 504 Teams – The school nurse as an essential team member (Position Statement). Author.
National Heart, Lung, and Blood Institute. (2023, November 21). Cystic fibrosis symptoms.
Nemours Children’s Health. (2018, June). Cystic fibrosis factsheet (for schools). Available at: https://kidshealth.org/en/parents/cf-factsheet.html
OSF HealthCare. (2024). Cystic fibrosis at school.
Shannon, R. A., & Kubelka, S. (2013). Reducing the risks of delegation: use of procedure skills checklists for unlicensed assistive personnel in schools, Part 2. NASN School Nurse (Print), 28(5), 222–226.
U.S. Department of Education. (2023). Frequently asked questions about Section 504 and the education of children with disabilities.
U.S. Department of Health and Human Services & U.S. Department of Education. (2008). Joint guidance on the application of the Family Educational Rights and Privacy Act (FERPA) the Health Insurance Portability and Accountability Act of 1996 (HIPAA) to student health records.
Wisconsin Department of Public Instruction. (2019). Meeting student health needs while on field trips. Tool kit for Wisconsin schools.
Yonkaitis, C. F., & Shannon, R. A. (2019). Health and education plans for students with special healthcare needs. In J. Selekman, R. A. Shannon, & C. F. Yonkaitis (Eds.). School nursing a comprehensive text. (3rd ed., p. 179). (Philadelphia, PA: F. A. Davis Company.
Reviewers
Renee Falkner, BSN, RN
School Nurse Supervision Specialist | Therapylog
Katherine Park, DNP, RN, NCSN
Nationally Certified School Nurse, Pierremont Elementary
Adjunct Professor, Maryville University School of Nursing
Last updated 4/18/2025
More Information
