Digestive
This resource provides current and comprehensive health care information for school health nurses. Related procedures, instructional videos and downloadable skills checklists can be searched by selecting the [More Information] button at the bottom of this web page.
Overview
Children may require an ostomy for various health conditions including Hirschsprung disease, inflammatory bowel disease such as Crohn’s disease, congenital anomalies, cancer, or as a result of trauma. The ostomy could be temporary (i.e., healing the intestines after surgery or trauma) or permanent. An ileostomy and colostomy are similar with the main difference being the segment of the intestines that is diverted to the abdominal wall. An ileostomy is an opening in the abdomen (stoma) in which a piece of the distal small intestine (ileum) is connected to the skin of the anterior abdominal wall and a colostomy is when the colon (large intestine) is connected to the skin of the anterior abdominal wall. The most common sections of the large intestine used for a colostomy are the descending or sigmoid colon with the less common being the ascending or transverse colon (United Ostomy Associations of America (UOAA), 2022). The student’s colostomy/ileostomy could be an end or loop ostomy. An end colostomy/ileostomy is created when the large or small intestine is brought to the abdominal wall. The end colostomy/ileostomy only has one round opening. A loop colostomy/ileostomy has two openings which are often oval. One of the openings is used for the removal of stool and the other to drain mucus. Loop ostomies are usually temporary (Potter, Perry, Stockert, and Hall, 2023).
Image: Colostomy Types
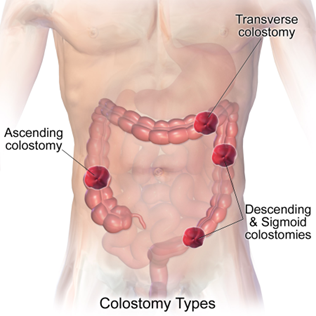
Source: Blausen.com staff, 2014
Stool Consistency:
The location of the ostomy will affect the consistency of the student’s stool. If the stoma is formed using the small intestine the stool will be more liquid in consistency. The lower into the large intestine will result in more formed stool:
- Ileum: output is the consistency of toothpaste
- Ascending colon: output is typically loose
- Transverse colon: output is pasty or soft like the consistency of oatmeal
- Sigmoid colon: output is typically normal in consistency
It would be important for the school nurse to discuss with the student and their parents/guardian what the student’s “normal stool consistency” is like.
Pouching Systems:
There are two categories of pouching systems, one-piece and two-piece pouching systems. For a one-piece system, the skin barrier and the pouch are attached together. A two-piece system consists of a separate skin barrier and pouch. A round plastic piece, also known as a flange, connects the two pieces by snapping together. Some two-piece systems are held together by adhesive. See the UOAA’s Types of Pouching Systems for more information.
Skin Care:
Protecting the skin around the stoma is vital. It is important to remember that stool contains digestive enzymes and these enzymes are irritating to the skin. One of the most important aspects of maintaining good skin integrity is ensuring that the student has well-fitting appliances to help prevent leakage of the stool. The most important part of the pouching system is the barrier which is also called the flange or the wafer. The barrier protects the skin from the ostomy output. The student’s barrier should create an effective seal that prevents the stool from leaking out under the barrier (Coloplast, 2022).
See the Coloplast Ostomy Education Table for images and descriptions of stoma and/or skin conditions.
Additional Equipment:
In addition to the pouching system the student may also use other supplies. The school nurse should review with the student and their parents/guardian which equipment and supplies the student uses. The school nurse should review their school district policies (if any) and request a health care provider’s order that addresses care and supplies required during school hours.
Table 1: Colostomy/Ileostomy Equipment
| Equipment | Description |
| Paste | Used to fill in creases or to help achieve a better seal |
| Rings | Used to fill in creases or valleys Helpful to make up for stoma irregularities and ensure a good seal to the skin Often easier to use than paste |
| Powder | Used to absorb moisture if skin is irritated or weeping |
| Adhesive remove wipes/spray | Clear sealant that goes over the skin after cleansing Used to seal skin before placing a skin barrier May also help with adhesion |
| Adhesive remover wipes/spray | Makes removal of skin barrier easier Helps remove any leftover adhesive |
| Belts | Can be used with pouching systems with belt loops Adjustable elastic belts may enhance the adherence and support pouching system |
Source: UOAA, 2022
The UOAA has developed Know Your Ostomy Supplies Checklist.
Ostomy Complications:
In addition to issues related to skin integrity one of the other concerns associated with ostomies is blockage. Blockage can occur if the student has eaten foods that are hard to digest (i.e., celery, citrus fruit, dried fruit, popcorn, raw fruits and vegetables, nuts or seeds, or meats with casing) or if the student has not been drinking enough fluids (Coloplast, 2019). The student may experience the following symptoms:
- Thin, clear liquid output with foul odor which can progress to no output
- Abdominal cramping near the stoma or throughout the entire abdomen
- Decreased urinary output
- Swelling of the abdomen or stoma (UOAA, 2020).
If the student were to experience these symptoms the school nurse or UAP should contact the student’s parents/guardian. The following steps are also recommended:
- If the student’s stoma starts to swell the pouching system should be replaced, making the wafer opening larger than normal to accommodate the swelling.
- If the student does not have any output from their stoma they should stop eating solids and drink only liquid, as long as they are not feeling nauseated or vomiting.
- Take short walks.
- Place a heating pad, on low, on their abdomen to help relax the abdominal muscles.
- Try different positions such as knee-to-chest, lying on their side (the side that has the stoma) with their knees bent as these positions may help to move the blockage forward.
- Massage the area around the stoma as most food blockages occur just below the stoma (UOAA, 2020).
The school nurse should discuss with the student’s parents/guardian and health care provider what steps to take if the student were to experience abdominal pain and/or decreased stool output. The following symptoms would be considered emergent:
- No stool output for several hours
- Abdominal pain
- Vomiting
- Distended abdomen
- Edematous stoma
- Darkened stoma (UOAA, 2020)
- Large amount of continuous bleeding (more than 4 tablespoons) in the pouch
- Deep cut in the stoma
- Repeatedly finding blood in the pouch or around the stoma edges (Coloplast, 2022).
As part of the school nurse’s planning process, they should discuss with the parents/guardian and health care provider what the plan of care should be if the student were to experience any of these symptoms at school (i.e., call parents and instruct them to take child to contact their child’s health care provider, call parents and instruct them to take the child to urgent care or the emergency department) (UOAA, 2020).
Although not emergent, the school nurse should assess the student’s stoma for the following issues:
- Discomfort, itching, soreness, or pain around the stoma
- Recurrent leakage under the pouching system or pouching system
- A bulge in the skin around the stoma
- A rash around the stoma that is red, or red with bumps
- Wart-like, pimple-like, or blister-like bumps under the skin barrier
- Any type of wound or scratch (UOAA, 2018)
The student’s Individual Health Care Plan (IHCP) should indicate what actions should be taken if the student were to experience these non-emergent symptoms. For more on IHCP see the Documentation section.
Delegation
There are a number of factors for the school nurse to consider when deciding whether to delegate this procedure to unlicensed assistive personnel (UAP). This section will provide a list of questions that the school nurse should answer to assist them in determining whether it is appropriate and safe to delegate the procedure. It is also important to remember that the questions related to delegation need to be answered for every individual student. The decision to delegate is based on circumstances related to the student, the nurse, the UAP, and the situation.
Questions to Ask to Inform Safe Delegation: The delegation questions below are based on the American Nurses Association’s Decision Tree for Delegation by Registered Nurses (ANA, 2012).
- Has the school nurse performed an initial assessment of the student to determine their needs?
The school nurse should not delegate the procedure to a UAP until they have completed the initial assessment. - Does school district policy, the school nurse’s job description, and the UAP’s job description allow procedures related to colostomy/ileostomy care to be delegated?
Although the Missouri Nurse Practice Act allows for registered nurses to delegate colostomy/ileostomy procedures, the district may have policies that prohibit or limit the school nurse’s ability to delegate. Additionally, the school nurse’s and UAP’s job descriptions may restrict delegation as well. - Is the school nurse competent to perform this procedure or does the school nurse need to acquire some knowledge or skills to be competent in this procedure?
If the school nurse is not competent or does not feel comfortable performing this procedure they should not delegate this procedure to a UAP. The school nurse must first acquire the necessary knowledge and skill to perform this procedure competently before they can delegate it to someone else. - Is the student’s condition stable? Is this an established colostomy/ileostomy or was it recently created? How predictable are the outcomes of the procedure?
A school nurse should not delegate colostomy/ileostomy procedures or care of the colostomy/ileostomy to a UAP if the student has a newly created ostomy. The outcomes are not predictable and thus the school nurse should perform the procedures until the student’s condition has stabilized. - Does the procedure require an initial or ongoing assessment to be performed during the procedure?
If an initial or ongoing assessment is required for the procedure to be performed, the procedure should not be delegated. - Does the UAP have the appropriate knowledge, skills, abilities, and willingness to perform the procedure?
All these factors need to be considered. Although a UAP may be competent to perform the procedure they may not be willing to do so and in that situation another UAP should be identified and trained. The registered nurse must retain responsibility for the procedure until training is complete. - Is there a procedure and/or protocol in place for this procedure?
A delegated nursing procedure must have an established sequence of steps that the UAP can follow. These steps should have a predictable outcome. The steps should be outlined in a written procedure or protocol. If the written procedure/protocol has not been developed, the school nurse should retain responsibility for the procedure until the procedure/protocol is in place. The procedure or protocol for colostomy/ileostomy care should include instructions on when the UAP should contact the school nurse and/or parents/guardians (i.e., change in consistency of stool, student complaining of abdominal pain, change in the color of the stoma, etc.). - Is the school nurse able to provide supervision to the UAP (direct or indirect depending on the situation)?
If the school nurse is not able to provide supervision, then the procedure should not be delegated. The school nurse will need to assess the situation to determine if direct or indirect supervision is required. The school nurse may also need to reassess the situation if the environment changes, for example, if the procedure is going to be performed during a time that the school nurse is not contracted to provide nursing services (i.e., over the weekend, during the summer, or if the school nurse is part-time). - Is the student ready to assume some responsibility for the procedure?
The school nurse should resume responsibility for the procedure since the school nurse is the only one who can initiate teaching. The school nurse would also want to observe the student performing the procedure to ensure that the student is competent. Once the school nurse has determined that the student is competent and can safely perform the procedure independently, they can delegate the supervision of the student to a UAP. If at a future date the school nurse is needed to teach the student additional skills, the school nurse would again need to resume responsibility for the procedure until the time in which the school nurse determined the student to be competent.
The Decision to Delegate:
There may be times when the school nurse and school administrator have conflicting opinions on the delegation of a procedure to a UAP. The school nurse may feel that delegation is not appropriate or the administrator may want the school nurse to delegate a procedure to an UAP that the school nurse feels is not competent. In these situations the school nurse may need to educate the administrator that the school nurse has a professional and legal responsibility to determine if delegation of a nursing procedure is appropriate and safe (ANA, 2012).
A resource developed by the National Association of School Nurses entitled, Fact Sheet for School Administrators, Families, and School Personnel: Nursing Delegation Requires the School Nurse may assist the school nurse in communicating with the school administration.
For continued learning see Navigating Delegation in the School Setting (PDF)
School Environment
Physical Environment:
An important component of care coordination for the student with a colostomy/ileostomy is access to a clean and private restroom. The UOAA has developed a Guideline for Ostomy Friendly Restrooms. It may be helpful for the student to have extra supplies at school and possibly more than one kit located in multiple locations (i.e., health room, main office, and/or student’s locker). It is recommended the student keep the following items in their extra supply kit:
- Extra ostomy bags
- Flange/wafer (if applicable)
- Scissors
- Tape
- Wipes
- Garbage bag (for soiled clothing)
- Plastic bag (to dispose of used ostomy bag)
- Extra set of clothes
(Patient Advisory Council for the ImproveCareNow Network, 2015)
Physical Education and Recess:
The school nurse should review the health care provider’s order to see if there are any restrictions associated with the student’s colostomy/ileostomy requiring activity restrictions or precautions during physical education class or at recess. The student may have a wrap or belt that they wear with their drainage bag when playing sports or engaging in activities where there may be more physical contact (Patient Advisory Council for the ImproveCareNow Network, 2015). The school nurse should review the student’s health care provider’s order and communicate with the student and their parents/guardians about any accommodations that are needed. For students who participate in swimming as a part of physical education, the UOAA has developed a Frequently Asked Questions document on using pool facilities.
Education of Peers and School Staff:
The school nurse should discuss with the student and their family about the student’s desire for the student’s peers and school staff to be made aware and educated about the student’s underlying health condition and/or need for a colostomy/ileostomy. Depending on the student and family’s wishes, educating peers may help alleviate endless questions and help teach peers on how to be supportive and inclusive. At a minimum, the student’s educational team should be educated about what signs and symptoms should be reported to the school nurse and parents/guardians. See Overview section for more information.
Students
An important first step when caring for a student who has a health condition that requires a colostomy/ileostomy would be to complete a health history and physical assessment, preferably with the student and their parents present.
Health History Questions: The school nurse may want to ask the student and their parents/guardians the following questions:
- Current health conditions
- Medications
- Allergies
- Previous hospitalizations and surgeries
- Most recent hospitalization
- Stoma shape
- Typical stoma color
- Stoma position (i.e., below skin level, flush to skin level, above skin level)
- Stoma location
- Stoma size
- Insurance coverage
- Health care provider(s) name and contact information
- Home health agency
- Preferred hospital, if applicable
The UOAA has developed a Know Your Ostomy Checklist.
Assessment Questions: The school nurse may want to consider asking the student and their parents/guardians the following additional questions:
- What is the student’s usual elimination pattern?
- What does the student’s stool usually look like?
- Does the student follow any certain routines to promote bowel elimination?
- How often does the student empty their ostomy pouch?
- What type of pouching system does the student use?
- Does the student use skin, odor, or other ostomy-related products?
- Does the student have any dietary restrictions or special needs?
- Does the student have any special considerations related to fluid intake needs?
- How does this health condition impact the student’s daily life?
- How often does the student miss school due to their health condition(s)?
- Tell me about your friends.
- How often do you spend time with them?
- Has the student shared information about their health condition(s) with their friends/peers?
- How independent is the student in the care of their ostomy and performing the ostomy procedures (i.e., emptying ostomy, care of the ostomy, skin care)?
- Does the student require activity precautions to prevent injury?
- Does the classroom environment support the student’s needs and/or equipment (i.e., desk/seating options, pass for bathroom or nurse)?
- What are the student’s and the parent’s goals associated with the care of their ostomy?
- Does the student and/or their parents have any concerns related to the student’s ostomy?
- What challenges does the student face in dealing with their health condition?
- Do you feel the student has been sufficiently supported by school staff in managing their health condition?
- Who has the student been going to when they need help?
- How often does the student have bad feelings about coming to school because they are worried/afraid/embarrassed about something (peers, assignments, teacher)?
- Has the student had to change any of their social activities because of their health condition?
- Has the student ever been picked on or bullied?
- Does the student have a 504 Plan or Individualized Education Program (IEP)?
- Would the student benefit from evaluations or assessments in any of the following areas: physical therapy, occupational therapy, speech and language therapy, assistive technology, adapted physical education, functional behavior, psychology, hearing and vision?
- Would the student benefit from additional academic support and/or modified education (i.e., copies of notes, extra time, reduced workload, simplified instructions, alternative formats for presentation of material, 504/IEP)?
- Does the student have an Individualized Health Care Plan (IHCP)?
- Is there a need for a specific plan for this student’s individual needs if there is a crisis in the building?
- If shelter-in-place were required or the school day needed to be unexpectedly extended, what additional supplies, equipment, and health care provider orders would be needed?
- How is the student transported to and from school?
- Does the student attend before or after school care?
- Does the student participate in school-sponsored clubs or athletics?
(Clarke, Embury, Yssel, 2014; Llorens, McKee, & Dempsey, 2020; Potter, Perry, Stockert, and Hall, 2023).
Transition Planning:
The school nurse should assess the student’s current and desired level of independence to determine what goals should be established for the student. Additionally, the school nurse should discuss with the student and family what steps have been initiated related to transition planning. The school nurse should consider including goals related to self-management and decision-making skills in the student’s Individualized Health Care Plan (IHCP) (NASN, 2019) and consider how those goals can be expanded upon each year to support independence, if appropriate. The UOAA’s Ostomy Self-Management Checklist might be a helpful resource to evaluate the student’s level of independence.
Transportation:
The school nurse should determine how the student is transported to and from school. Although an emergency related to the student’s colostomy/ileostomy is unlikely, the school nurse, the student, and their family should discuss whether informing the bus driver of the student’s health condition and colostomy/ileostomy is necessary.
Communication
It is important for the school nurse to discuss with the student and their family the best way(s) to communicate with them. Does the parents/guardian have a preference (i.e., email, text, telephone call)? Do the parents prefer to have the communications sent to both parents or is there a parent who manages the communication with the school nurse?
The school nurse may want to consider having the parents/guardians complete a Health Insurance Portability and Accountability Act (HIPAA) compliant medical release form to facilitate communication with the student’s health care team. Although HIPAA does not require parental consent to allow the school nurse to discuss the student’s treatment plan, such as medications and nursing procedures, with the student’s health care provider, having a signed consent form would undoubtedly make the process go smoother for all involved parties (U.S. Department of Health and Human Services & U.S. Department of Education, 2008).
NASN-FERPA-HIPAA-CONSENT-SAMPLE
Medication
Health Care Provider Order: There are not typically medications associated with the colostomy/ileostomy itself. The student may be prescribed medications for other health conditions associated with the need for the colostomy/ileostomy. If these medications are administered at school an order from a health care provider would be required.
If the student applies skin barrier powders, pastes or other skincare products the school nurse should review their school district policy to determine if an order from a health care provider is needed for these products to be applied by the school nurse, UAP, or the student themself.
There may be times when the student’s stoma is irritated or infected and a topical medication is prescribed. If this medication is to be applied at school, the school nurse would need an order from a health care provider. The order should include:
- The student’s name
- Date of birth
- Name of the medication
- Dose
- Route
- Time of administration
- Reason for administration
MO DHHS Medication Manual – includes Six Rights of Medication Administration
Field Trips
Field trips and other out-of-school activities will require some planning by the school nurse. There are several variables that the school nurse will want to consider and plan for, including:
- Does the student require someone to accompany them on the trip to care for their colostomy/ileostomy or are they independent in these cares?
- If the student does require someone to assist with the procedure(s) and/or care of the colostomy/ileostomy, who will accompany the student on the field trip to perform necessary procedures?
The individual who will be providing the care or performing the procedure must have the knowledge, ability, skills, and willingness to perform the procedure (Erwin, Clark, & Mercer, 2014). - Where will the colostomy/ileostomy supplies be stored?
It is important to have all needed supplies readily available. Supplies should not be left on the bus but should be with the student at all times. - How will the student’s privacy be protected?
The school nurse should discuss with the student and their family where the procedure(s) will be performed during the field trip and the student and family’s expectations related to privacy (i.e., the student may not have access to a private bathroom). - How will safety and cleanliness be ensured?
In addition to privacy, the school nurse must think through possible scenarios on where the procedure may be performed and what additional precautions and supplies may be needed to ensure safety and cleanliness. - How will the procedure be documented?
Timely documentation is a key component of nursing. The school nurse should consider how procedures and medication administration, if applicable, that occur on a field trip will be documented (Erwin, Clark, & Mercer, 2014; NASN, 2021). - Is the field trip occurring out of state or out of the country?
Field trips that occur out of the student’s home state will require some additional planning. If the school nurse will be accompanying the student on the field trip, they will want to determine if the state(s) that will be traveled through or visited are a part of the Nurse Licensure Compact. If the school nurse will not be accompanying the student but instead will be delegating the procedures, the school nurse will want to review the other state’s nurse practice acts and associated rules and regulations to determine if the procedure can be delegated to a UAP in that state.
For out of the country field trips, the school nurse should discuss with school administration any applicable laws to determine what additional steps may be needed. In addition, the U.S. Embassy can provide information on points of contact for destination countries. The school will also want to connect with the student’s parents/guardians regarding informing the Transportation Security Administration about the student’s health needs.
(Erwin, Clark, & Mercer, 2014; NASN, 2019; Wisconsin Department of Public Instruction, 2019).
It is important to note that the Section 504 of the Rehabilitation Act does not allow for a student with a disability to be excluded from a field trip due to their disability.
Documentation
Health Care Provider Order: For students who require colostomy/ileostomy care at school, the following information should be included in the health care provider’s order:
- Student’s name
- Date of birth
- Type of ostomy
- Colostomy/ileostomy materials used including brand and type of bag, stoma size
- Products used for skin care/skin breakdown
- Products used for odor
- Level of independence the student has with performing the procedure(s) (i.e., fully independent, needs assistance, or fully dependent)
- When the health care provider would like to be contacted
- What constitutes an emergency
- Steps to take in response to colostomy/ileostomy emergency
(Kennedy Krieger, 2020)
Emergency Action Plan: The school nurse may want to consider developing an Emergency Action Plan that outlines the steps to take if certain symptoms (i.e., edematous or darkened stoma, abdominal distention, excessive blood in the stool, vomiting). The school nurse should consult with the parents/guardian and health care provider to determine what signs and symptoms should be included in addition to the steps to be taken if the symptoms were present.
Parent/Guardian Authorization: In addition to the health care provider’s order, the school nurse will also need written authorization from the parents/guardians to perform colostomy/ileostomy procedures at school. The authorization form can be a separate document that just the parents sign or a document can be developed that combines the health care provider’s order and parent authorization in one form.
Procedures and Medication Administration: All medication administration and colostomy/ileostomy related procedures will need to be documented, whether they are performed by the school nurse or the UAP. Many times the medication administration and procedures are documented in the student’s health record. The school nurse will also want to ensure that medications being administered or procedures being performed during field trips, before or after school, and/or during any school-sponsored activities are being documented. If the student is independent in their care of their ostomy, the school nurse should review their school district’s policies, procedures, and/or protocols to determine if the student’s self-care of their ostomy needs to be documented in the student’s health care record.
Staff Competency Validation: If the procedures or medication administration is delegated to a UAP the school nurse should document that the UAPs knowledge, abilities, and skills have been assessed. Many times these factors are documented on a skills competency checklist (see Just in Time resources > Digestive > downloadable skills checklists). There should be a place on the skills competency checklist for the school nurse and UAP to sign to indicate that they feel competent and are willing to perform the procedure. Once the procedure has been delegated the school nurse is responsible for periodic evaluation of the UAP and their competency. The school nurse must determine how often the supervision is needed. After the school nurse has re-evaluated the UAP’s competency, they should document the date of the evaluation (Shannon & Kubelka, 2013; Selekman & Ness, 2019). The school nurse should organize the competency documentation in a way that easily allows them to determine when subsequent evaluation and documentation of competency is needed. For more information on delegation see the Delegation section.
Individualized Health Care Plan (IHCP): IHCPs should outline the plan of care for the student, including but not limited to:
- Actions the school nurse will take to support the student’s educational attainment
- The education and training that will be provided to school personnel
- The development of Emergency Action Plans, including steps to be taken in case of an evacuation
- And the accompanying expected outcomes for each of the nursing interventions (NASN, 2020).
Section 504 Plan: Students with a colostomy or ileostomy may qualify for a Section 504 Plan since their health condition may impact a major life activity, which includes the functioning of major bodily systems such as the gastrointestinal system. If the student has been identified as qualifying for a 504 Plan, the school nurse may be involved in identifying appropriate accommodations and writing the plan. Once developed, the school nurse will want to frequently review, update, and document in the 504 Plan (NASN, 2020). For more information on Section 504 Plans see Legal Issues section.
Procedure
Links to Just in Time procedures > Digestive
Emergency Preparedness
Shelter-in-Place and Other Emergency Events: In addition to an Emergency Action Plan (see Documentation section), the school nurse must also plan for other potential emergencies such as lockdown, extreme weather events, evacuations, and shelter-in-place events. To develop plans to address these possible emergencies the school nurse would want to collaborate with other school staff and administrators. The emergency preparedness plan should address the following:
- Location of extra supplies in case of lock-down.
- Provision of supplies that may be needed if there is no access to a restroom, including supplies that will be needed to address the lack of privacy.
- Access to extra colostomy/ileostomy supplies in case of unplanned extended school day or shelter-in-place.
For more information on emergency planning see Missouri School Boards’ Association’s Emergency Planning Guide for Students and Staff with Special and Functional Needs within Schools.
Legal Issues
Section 504 Plan: Students with a colostomy or ileostomy may qualify for a Section 504 Plan. Section 504 of the Rehabilitation Act of 1973 as amended through the Americans with Disabilities Amendment Act (ADAA) in 2008 ensures that students who have disabilities have access to a free and appropriate public education (FAPE) (U.S. Department of Education, 2023). FAPE provides a student with a physical or mental impairment that impacts one or more major life activities, which includes the functioning of major bodily systems such as the gastrointestinal system, with related services and accommodations in the general education classroom (U.S. Department of Education, 2023; NASN, 2023). If the student does not have a 504 Plan the school nurse should determine if an evaluation is indicated (see Students section for questions to ask student and family to determine if 504 or IEP evaluation is indicated). If it is determined that the student qualifies for a Section 504 Plan, the school nurse may want to consider the appropriateness of the following accommodations:
- Allow the student to use the restroom whenever there is a need, without needing to ask for permission.
- Allow the student to leave class early or arrive late without being penalized.
- The option for the student to use a private restroom.
- The student will have the option to store additional supplies, including a change of clothing, in the private restroom.
- Academic support if they miss class due to health concerns (including health care provider appointments, hospitalization, or illness).
- Permission to use a water bottle at all times.
- The provision of necessary accommodations on field trips and other school sponsored activities.
- There will be “stop the clock testing.” “Stop the clock testing” means that, when the student is taking an exam, if he/she needs a bathroom break or a break due to pain, the time for completing the test will be extended by the amount of time the student spends away from the testing room. This accommodation shall be provided without penalty and shall apply to all tests including but not limited to State Standardized Testing and course exams (Crohn’s and Colitis Foundation, 2023).
The Crohn’s and Colitis Foundation has created a Section 504 Plan template.
Resources
Peristomal Skin Assessment Guide for Clinicians
Coloplast Ostomy Education Table
Pull Thru Network Glossary of Terms
Guidelines for Ostomy Friendly Restrooms
References
American Nurses Association. (2012). Principles of delegation.
Blausen.com staff. (2014). Colostomy types. WikiJournal of Medicine 1 (2). DOI:10.15347/wjm/2014.010. ISSN 2002-4436
Clarke, L.S., Embury, D.C., and Yssel, N. (2014). Supporting students with disabilities during school crisis. A teacher’s guide. Teaching Exceptional Children, 46(6), 169-78.
Coloplast. (2019). Life after your child’s ostomy.
Coloplast. (2022). Teen life with an ostomy.
Crohn’s and Colitis Foundation. (2023). Template section 504 plan for children with inflammatory bowel disease.
Erwin, K., Clark, S., & Mercer, S.E. (2014). Providing health services for children with special health care needs on out-of-state field trips. NASN School Nurse, 29(2), 84-8. doi: 10.1177/1942602X13517005
Francone, T. D. (2023, April 24). Overview of surgical ostomy for fecal diversion. UpToDate.
Kennedy Krieger. (2020). Ostomy.
Llorens, A., McKee, S., & Dempsey, A.G.). (2020). In A.G. Dempsey (Ed.). Pediatric health conditions in schools. (pp. 26-27). New York, NY: Oxford Press.
National Association of School Nurses. (2019). Transition planning for students with healthcare needs (Position Statement). Silver Spring, MD: Author.
National Association of School Nurses. (2020). Understanding student health and education plans.
National Association of School Nurses. (2021). Medication administration clinical practice guidelines in the school. Author.
Patient Advisory Council for the ImproveCareNow Network. (2015). The ostomy toolkit. Gutsy living with a little gutsy help.
Potter, P. A., Griffin Perry, A. G., Stockert, P. A., & Hall, A. (2023). Chapter 47 Bowel elimination. In Fundamentals of Nursing. (11th ed.). (pp. 1276-1317). St. Louis, MO: Elsevier.
Selekman, J. & Ness, M. (2019). Students with chronic conditions. In J. Selekman, R.A. Shannon, C.F. Yonkaitis, (Eds.). School nursing, a comprehensive text (3rd ed., p 493). Philadelphia PA.: F. A. Davis Co.
Shannon, R. A., & Kubelka, S. (2013). Reducing the risks of delegation: Use of procedure skills checklists for unlicensed assistive personnel in schools, Part 2. NASN School Nurse (Print), 28(5), 222–226.
United Ostomy Associations of America. (2018, December 11). Peristomal skin complications- Potential causes and what to do.
United Ostomy Associations of America. (2020). How to treat ileostomy blockage.
United Ostomy Associations of America. (2022). Living with a colostomy.
United Ostomy Associations of America. (2023). Ileostomy facts.
U.S. Department of Education. (2017, May 2). Sec. 300.34 related services.
U.S. Department of Education. (2018, May 25). Sec. 300.8 Child with a disability.
U.S. Department of Education. (2023). Frequently asked questions about Section 504 and the education of children with disabilities.
U.S. Department of Health and Human Services & U.S. Department of Education. (2008). Joint guidance on the application of the Family Educational Rights and Privacy Act (FERPA) the Health Insurance Portability and Accountability Act of 1996 (HIPAA) to student health records.
Wisconsin Department of Public Instruction. (2019). Meeting student health needs while on field trips. Tool kit for Wisconsin schools.
Reviewers
Renee Falkner, BSN, RN
School Nurse Supervision Specialist | Therapylog
Katherine Park, DNP, RN, NCSN
Nationally Certified School Nurse, Pierremont Elementary
Adjunct Professor, Maryville University School of Nursing
Last updated 4/18/2025
More Information
